
Overview
Heel spurs are a common foot problem resulting from excess bone growth on the heel bone. The bone growth is usually located on the underside of the heel bone, extending forward to the toes. One explanation for this excess production of bone is a painful tearing of the plantar fascia connected between the toes and heel. This can result in either a heel spur or an inflammation of the plantar fascia, medically termed plantar fascitis. Because this condition is often correlated to a decrease in the arch of the foot, it is more prevalent after the age of six to eight years, when the arch is fully developed.
Causes
Causes of Heel Spur Syndrome are mostly due to your foot structure. Foot structure is due to hereditary for the most part, meaning it was the way you were when born. Other factors such as increase in weight, injury, improper shoes, or different activities may change the way your foot functions as well. If one leg is longer or shorter than the other, this may make your foot function improperly and be the cause of the heel spur syndrome. Improper shoes may be ones that are new or ones that are worn out and do not give good support. The higher priced shoes do not mean it's a better shoe. Pronation is a term used to describe a foot which allows the arch to fall more than normal and allows for the fascia along the bottom of the foot to put a tighter pull or a different angle of pull on the heel bone. Over time, this constant pull of the tight fascia can force the bone to enlarge and form a spur. It is not the heel spur that causes the pain directly. The spur may cause pressure against a nearby nerve causing a neuritis, or a bursa causing a bursitis.

Symptoms
Most bone spurs cause no signs or symptoms. You might not realize you have bone spurs until an X-ray for another condition reveals the growths. In some cases, though, bone spurs can cause pain and loss of motion in your joints.
Diagnosis
Sharp pain localized to the heel may be all a doctor needs to understand in order to diagnose the presence of heel spurs. However, you may also be sent to a radiologist for X-rays to confirm the presence of heel spurs.
Non Surgical Treatment
In extreme cases, a doctor may recommend surgery for the removal of heel spurs. Fortunately, this is the exception rather than the rule. Most cases can be resolved with a combination of icing, rest, foot stretches and supporting the foot with an orthodic shoe insert specifically designed for this condition. We recommend that you continue on to our article on Heel Spur Treatment to discover the best, speediest and most affordable methods of resolving this ailment without invasive medical procedures.
Surgical Treatment
In a small number of cases (usually less than 5 percent), patients may not experience relief after trying the recommendations listed above. It is important that conservative treatments (such as those listed above) be performed for AT LEAST a year before considering surgery. Time is important in curing the pain from heel spurs, and insufficient treatment before surgery may subject you to potential complications from the procedure. If these treatments fail, your doctor may consider an operation to loosen the plantar fascia, called a plantar fascia release.
 Overview
Overview Symptoms
Symptoms





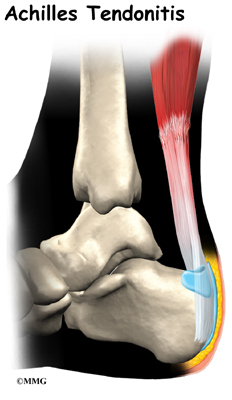 The Achilles tendon attaches the calf muscle to the heel bone. Jumping, climbing and strenuous exercise can strain the tendon and calf muscle, which can cause the type of inflammation known as tendinitis. This injury can be mild enough that it can be treated by over-the-counter medications or so severe that it must be repaired surgically. Chronic tendinitis can cause microscopic tears in the muscle which can weaken the tendon and increase the risk for tear or rupture. Symptoms usually include pain and swelling near the ankle. Pain may lead to weakness in the area that increases with walking and running. Stiffness in the tendon may be worse in the morning.
The Achilles tendon attaches the calf muscle to the heel bone. Jumping, climbing and strenuous exercise can strain the tendon and calf muscle, which can cause the type of inflammation known as tendinitis. This injury can be mild enough that it can be treated by over-the-counter medications or so severe that it must be repaired surgically. Chronic tendinitis can cause microscopic tears in the muscle which can weaken the tendon and increase the risk for tear or rupture. Symptoms usually include pain and swelling near the ankle. Pain may lead to weakness in the area that increases with walking and running. Stiffness in the tendon may be worse in the morning.
 The Achilles tendon connects the muscles in the back of your lower leg to your heel bone. It allows you to move your foot down (step on the gas motion). This movement is essential for walking, running, and jumping. A sudden strong contraction of the lower leg (such as when playing sports) can partially tear or rupture the Achilles tendon. This injury is more likely if there is prior injury or inflammation of that tendon from prior stress. You may feel a pop or snap, or like you have been kicked. An Achilles tendon tear will cause local swelling and pain and difficulty in walking. A complete Achilles rupture is usually treated with surgery to attach the torn ends of the tendon. This is followed by 6-8 weeks in a walking cast, boot, or splint. Nonsurgical treatment is an option, but it will take longer to heal and the risk of repeat rupture is greater. With either type of treatment, you will need a physical therapy program to strengthen your Achilles tendon. It will take 4-6 months to return to your former level of activity.
The Achilles tendon connects the muscles in the back of your lower leg to your heel bone. It allows you to move your foot down (step on the gas motion). This movement is essential for walking, running, and jumping. A sudden strong contraction of the lower leg (such as when playing sports) can partially tear or rupture the Achilles tendon. This injury is more likely if there is prior injury or inflammation of that tendon from prior stress. You may feel a pop or snap, or like you have been kicked. An Achilles tendon tear will cause local swelling and pain and difficulty in walking. A complete Achilles rupture is usually treated with surgery to attach the torn ends of the tendon. This is followed by 6-8 weeks in a walking cast, boot, or splint. Nonsurgical treatment is an option, but it will take longer to heal and the risk of repeat rupture is greater. With either type of treatment, you will need a physical therapy program to strengthen your Achilles tendon. It will take 4-6 months to return to your former level of activity.
